Data drives decisions, evidence-based decisions.
Yet, in the world of breathtakingly fast data analytics, how can you be certain that only the right people are seeing sensitive data? This is the purpose of Role-Based Control Access (RBAC) also known as Role-Based Security (RBS).
What is Role-Based Access Control (RBAC)?
Each person in an organization has a position or a role. RBAC sets a framework whereby each employee only has access to data that is pertinent to that role. If the individual has responsibility for budget decisions for a specific department, he/she has access to that data only and no access to other departments.
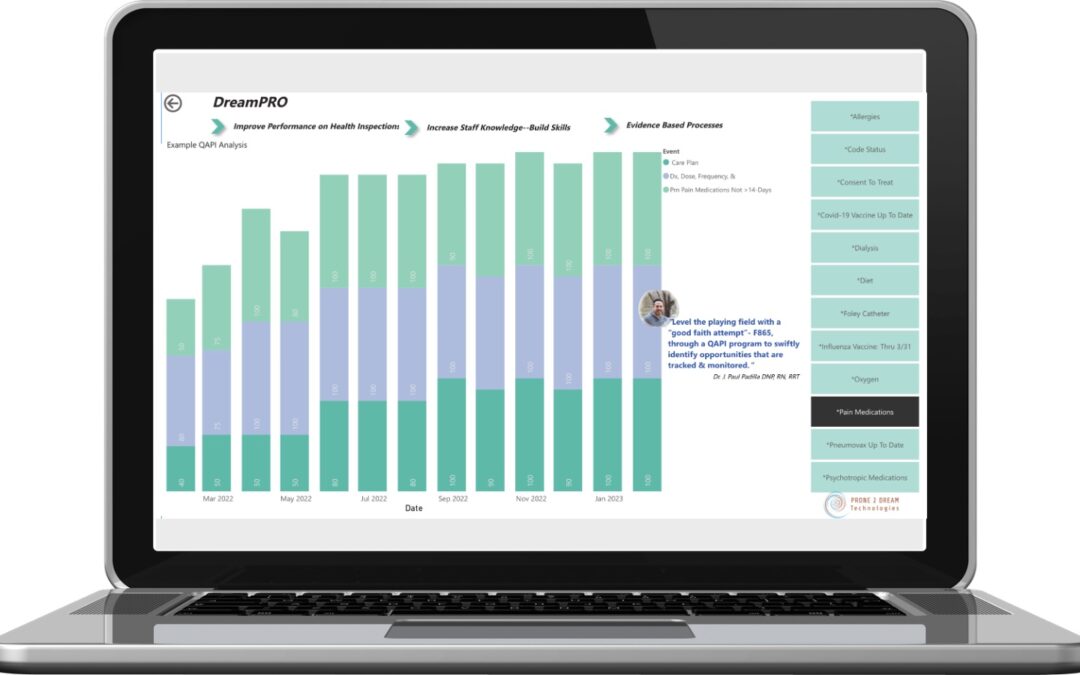
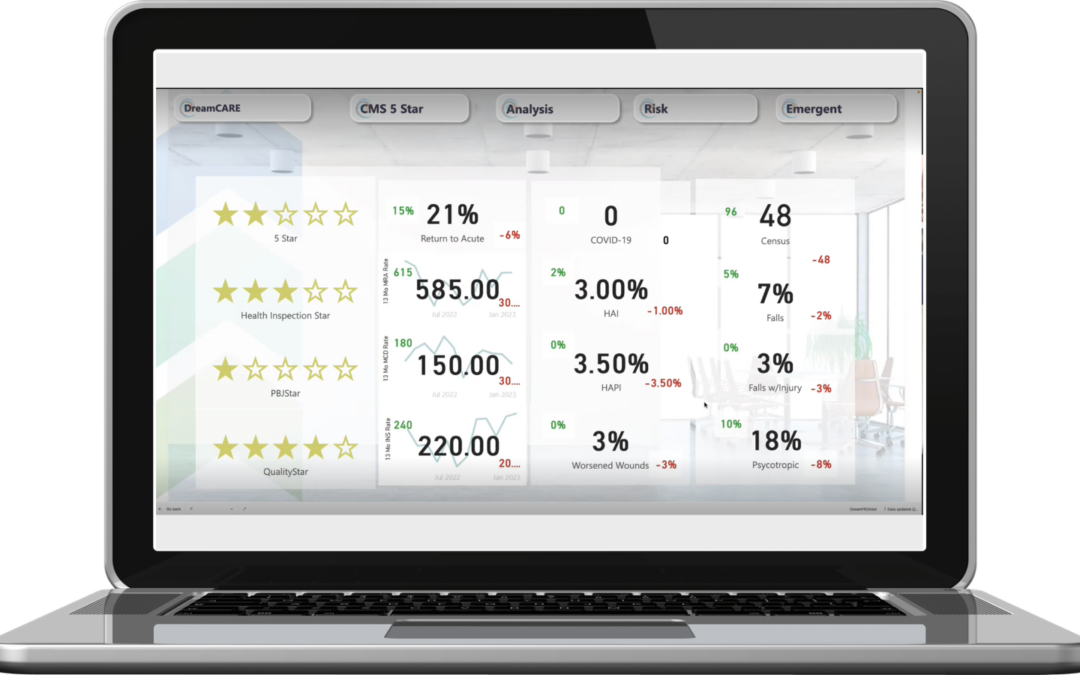
Prone 2 Dream Technologies deploys RBAC for its DreamCORE Dashboards. Skilled Nursing business intelligence is delivered in drillable dashboards with a focus on Census, Overtime, Receivables, and Expenses. These are the CORE of the business and where frontline department leaders are making decisions about how to spend the company’s revenue.
These leaders are expected to contribute to the overall profitability of the company. However, they typically have to wade through data overload by signing into multiple platforms or shuffling multiple spreadsheets to find what they need to make decisions.
DreamCORE Dashboards presents the plethora of skilled nursing data in a logical, relevant format, with infinite views. RBAC narrows the scope to each individual’s frame of reference – he or she only sees the data for areas where they can make an impact. They get the data they need… and ONLY the data they need.
Here’s the RBAC framework for DreamCORE Dashboards:

Examples of Role-Based Access Control
Culinary Manager – Sees payroll, overtime, and department budget adjusted daily per fluctuating census only for the facility’s culinary department
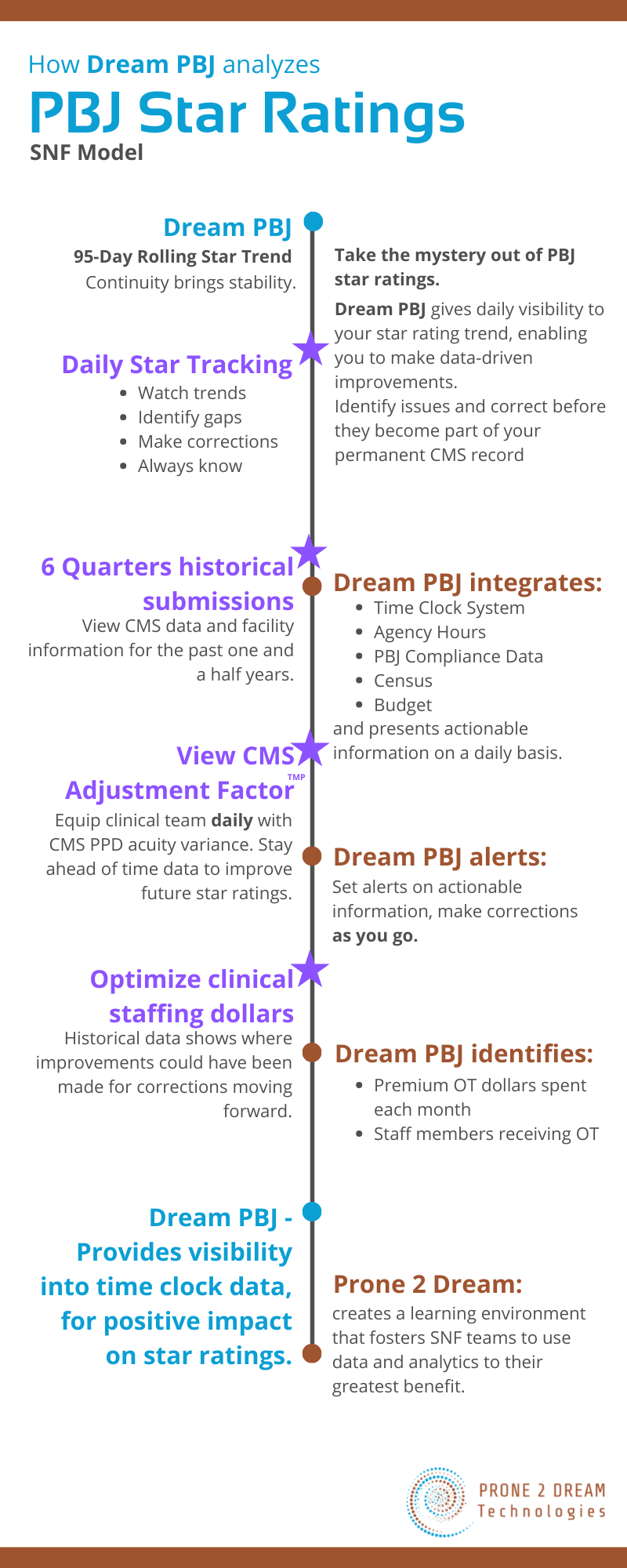
Director of Nursing – Sees payroll, overtime, and department budget adjusted daily per fluctuating census only for the facility’s nursing department. Plus, she sees a daily tracking of her CMS PBJ star rating – data only relevant to her role.
Facility Administrator – Sees all the data relevant to that specific property/location.
Regional Director – Sees all the data for the facilities he oversees.
Executive Team – All the data for all the facilities, as well as corporate financials, P&L, forecasts, Payroll Analysis, and more.
As a result, sensitive data remains secure, and each individual is aware that their focus is different from another within the company. Yet DreamCORE Dashboards provide one version of the truth, updated daily.
Two individuals in different roles, but who have access to the same dashboard page are both seeing the same data. For example, a regional director has a virtual meeting with a facility administrator. They are both seeing that facility’s “green data” – one version of the truth, updated daily.
Benefits of RBAC in DreamCORE Dashboards
- Protects sensitive payroll data. Most department leaders need to control schedules and overtime expense, yet need to keep wage rates secure. DreamCORE Dashboards provides that security while allowing leaders to make data-driven decisions.
- Protects patient data. DreamCORE Dashboards focus on the financial data of a patient’s stay and it’s only available to certain roles, as defined by executive leadership.
- Eliminates data overload at the front line. Narrowing the focus is the first step towards positive outcomes – DreamCORE Dashboards are a tool for front line success.
- Ease of change. Individuals’ roles change – whether they are adding responsibilities, moving to a different facility, or getting a promotion, changing access is as easy as contacting our support team.

The Ease of Single Sign-on
Nobody needs yet another set of login credentials to gain access to their data. Prone 2 Dream is a Microsoft Partner, so with your current Microsoft account, your team simply logs in to their email account and access to their dashboards is a click away.
Our single sign-on feature mitigates the risk in accessing third-party sites, reduces time spent accessing multiple accounts, lowers the total cost of ownership of IT with fewer help desk / support ticket requests, and creates happy users.
Empower your front line leaders
Data drives decisions. If your facilities are wading in data overload or simply don’t have the time to shuffle through their various papers and platforms, book a demo of DreamCORE Dashboards today.
We understand that data can be intimidating, especially to department managers who were hired for their acumen in distinctly different areas. We take pride in providing onboarding and training for your teams and helping them learn to love their numbers.